- Conditions
- Prepatellar bursitis
Prepatellar bursitis Housemaid’s knee / bursitis in the front of the knee
Introduction
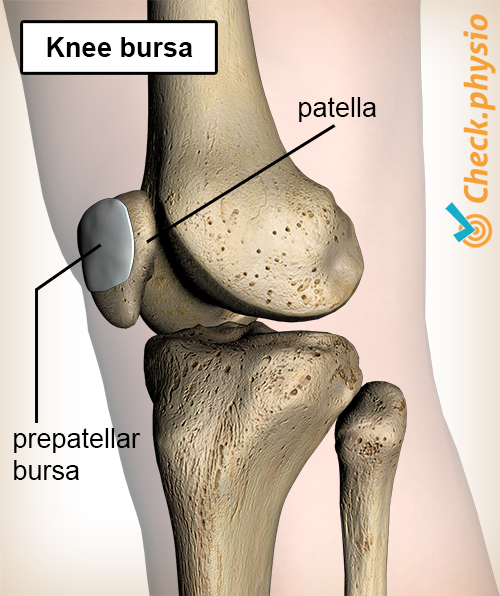
In case of prepatellar bursitis, the bursa at the front of the knee is inflamed. This bursa is located between the skin and the kneecap.
Prepatellar bursitis can be caused by an infection or result from excessive straining or bumping the knee. Symptoms include pain, redness, warmth and swelling of the knee. Because the condition is more common in people who sit on their knees a lot, prepatellar bursitis is sometimes also referred to as housemaid’s knee
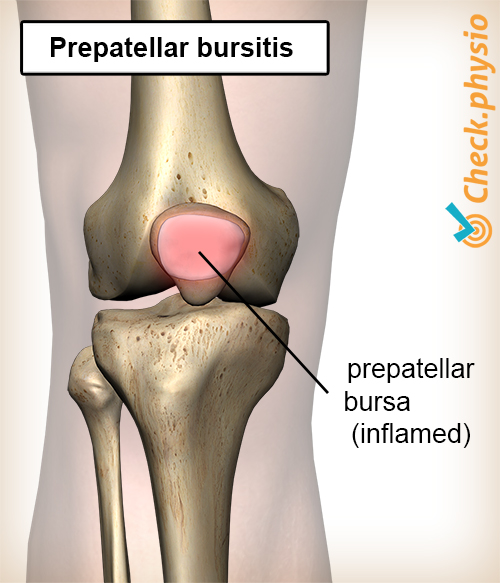
Description of the condition
A olecranon bursitis of the elbow.
When inflamed, the bursa becomes filled with fluid and gets thicker and painful. The skin above often also feels warmer and turns red.
Cause and origin
Prepatellar bursitis can develop because work activities or sports require someone to sit on the knees a lot, or when (repeatedly) falling on the knees. Think of road workers or people who play judo.
It is also possible that an infection is the culprit. That’s when bacteria enter the bursa through a wound on the knee and cause an inflammation there.
When prepatellar bursitis suddenly develops, this is referred to as acute bursitis. If the inflammation lasts a long time, or (regularly) recurs, this is referred to as chronic bursitis.
Signs & symptoms
Symptoms that can develop with prepatellar bursitis are:
- Pain that worsens when pressing or bearing weight on the bursa (tenderness on the kneecap).
- Local swelling of the kneecap.
- Redness and warmth of the knee.
- Limitation of, in particular, knee flexion.
- In case of an infection, a small wound may be visible and a fever may occur.
Diagnosis
An interview with a doctor or physiotherapist will focus on finding out what the symptoms are and how they arose. This is followed by a physical examination in which local inflammatory symptoms such as pain, redness, warmth and swelling are examined. Based on this, prepatellar bursitis can be diagnosed.
The suspicion of infectious bursitis is confirmed when the knee is very red and the symptoms developed after an injury. To be sure, some fluid can be aspirated from the bursa with a needle to be tested.
Treatment and recovery
To let the bursitis heal, it is important to give the knee some rest. This means that pressure on the knee should be avoided as much as possible. Sparing the knee temporarily usually leads to spontaneous healing.
A doctor can opt to drain the bursa with a syringe. This usually gives immediate relief from the pain. Unfortunately, there is a chance that the bursa will swell up again afterwards. A painkiller and anti-inflammatory can remedy the complaints of chronic bursitis that do not result from an infection. However, when there is an infection, antibiotics will be prescribed.
When the above advice and treatments do not help, the bursa can be surgically removed.
More info
You can check your symptoms using the online physiotherapy check or make an appointment with a physiotherapy practice in your area.
References
Magee, D.J. (2014) Orthopedic physical assessment Elsevier saunders: St. Louis.
Knuistingh Neven, A. & Eekhof, J.A.H. (2005) Bursitis olecrani en bursitis prepatellaris Huisarts & Wetenschap. 48(5):mei:2005.
Magee, D.J., Zachazewski, J.E., Quillen, W.S., Manske, R.C. (2016) Pathology and intervention in musculoskeletal rehabilitation Elsevier, 2nd edition.